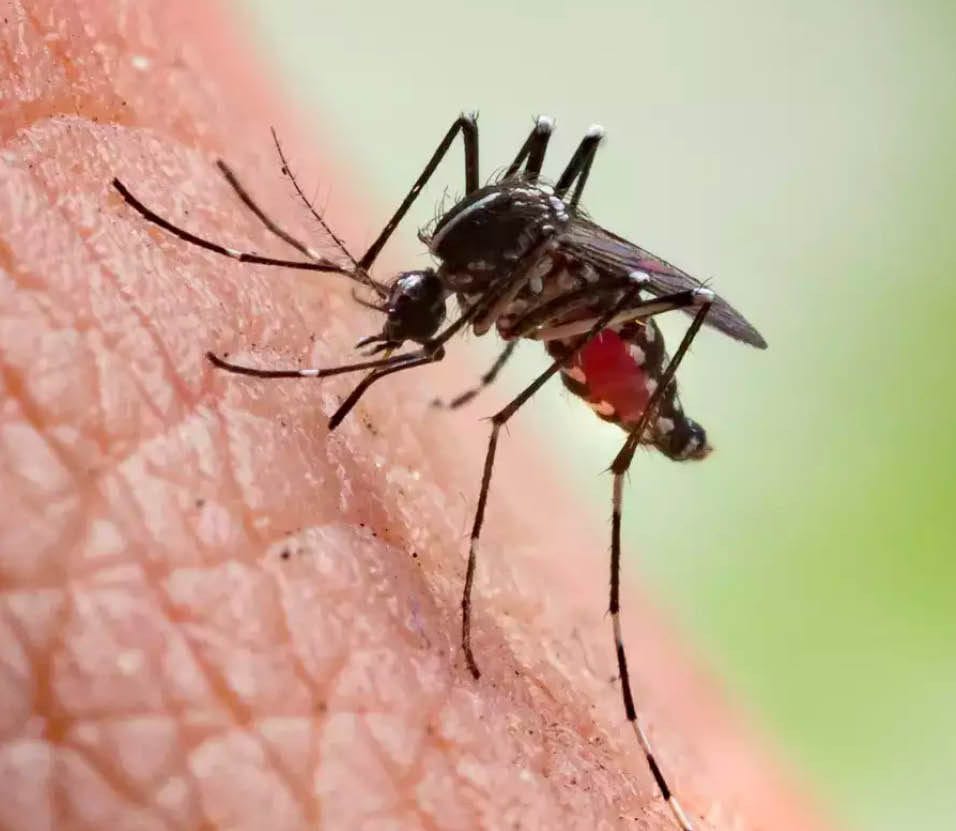
Malaria, a life-threatening disease transmitted through mosquito bites, has plagued various regions of the world for centuries. While significant progress has been made in combating this deadly illness, it continues to pose a threat to many tropical countries, including the Maldives. This article delves into the reality of malaria in the Maldives, a nation renowned for its breathtaking beauty and pristine beaches. Known colloquially as "Malayria," this unique blend of the words "Maldives" and "malaria" signifies the persistent fight against the disease within the archipelago. By exploring the history, impact, prevention, and ongoing efforts to eliminate malaria in the Maldives,
Welcome to Town Pharmacy, Rawalpindi. Your One Stop Shop For Geniune Medicine, Delivered All Over Pakistan
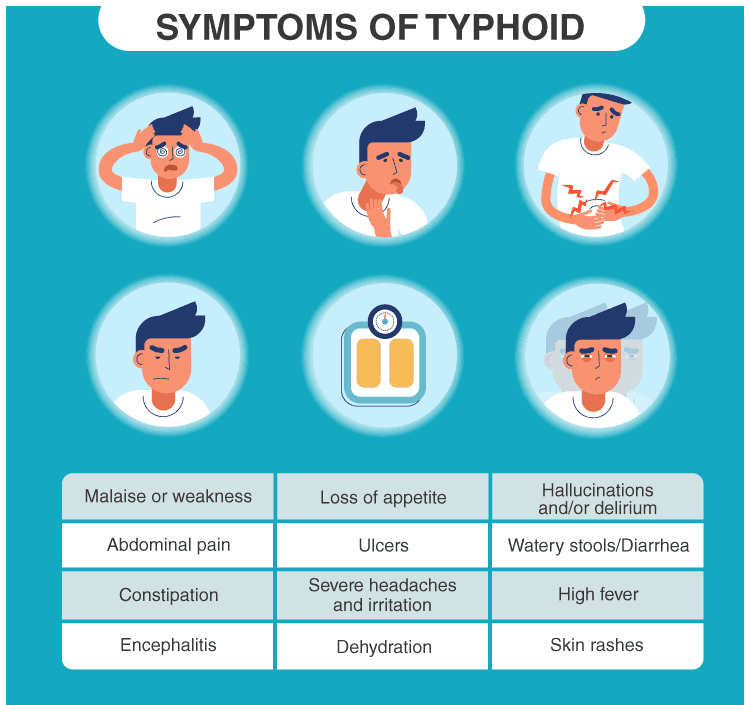
Typhoid fever is a bacterial infection caused by Salmonella enterica serotype Typhi (S. Typhi) bacteria. It is a significant global health concern, particularly in areas with poor sanitation and limited access to clean water. In this blog post, we will explore the causes, symptoms, diagnosis, treatment, medication, dosage, and prevention strategies for typhoid fever. By understanding this disease and its management, we can take necessary precautions and promote better public health practices.