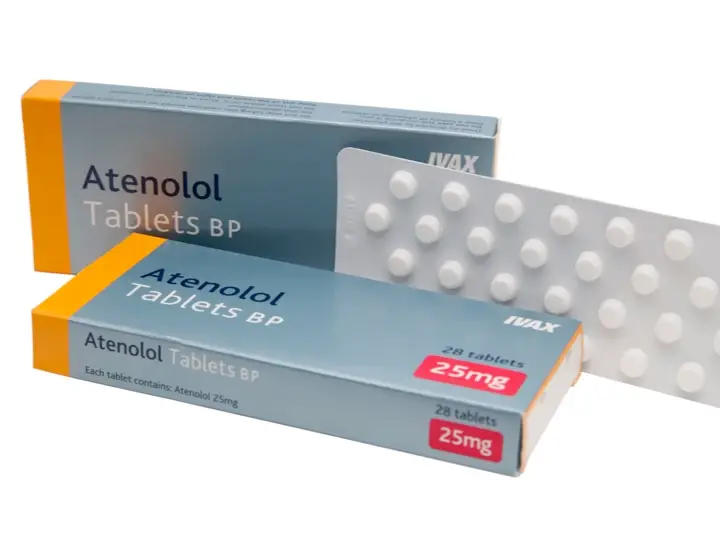
Ibuprofen available under brand name of Brufen is a common pain reliever used to treat a variety of aches and pains, such as back pain, period pain, and toothache. It also helps with inflammation from strains and sprains, as well as arthritis discomfort.
Welcome to Town Pharmacy, Rawalpindi. Your One Stop Shop For Geniune Medicine, Delivered All Over Pakistan
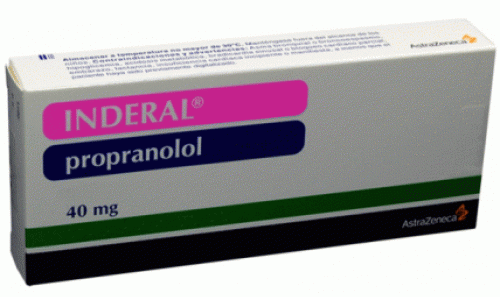
Propranolol, available under the brand name of Inderal is a non-selective beta adrenergic antagonist is used to treat a variety of conditions, including hypertension, angina, atrial fibrillation, myocardial infarction, migraine, essential tremor, and hypertrophic subaortic stenosis.
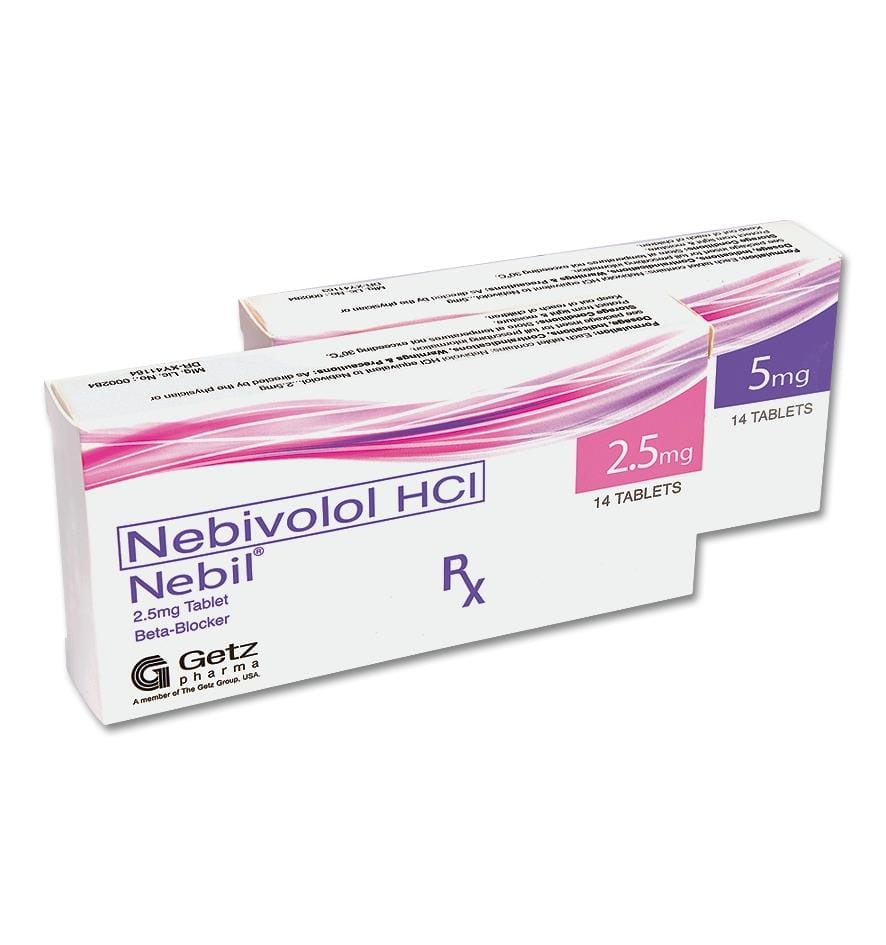
Nebivolol a novel beta blocker, available under the brand names of Nebil, Nebix and Byvas etc. is more selective for beta1-adrenergic receptors than other drugs in this class and has a unique, not found in other beta-blockers now available to doctors, nitric oxide (NO)-potentiating, vasodilatory effect.